Parotid Gland Definition
The parotid gland is one of three salivary glands contained within the human body. The same applies to many animals. It is the largest of the three glands and the biggest producer of saliva. Saliva has lubricating and digestive properties that help protect the alimentary canal linings during meals.
Parotid Gland Overview
The saliva secretion itself is very “serous,” or protein-rich, compared to the saliva expelled from the other salivary glands. This will of course aid in the parotid gland’s principal functions. Saliva also has antibacterial properties, which protect the tooth enamel from being broken down by bacteria. One of the main proteins secreted by the glands is amylase. This enzyme is responsible for breaking down starches as they enter the mouth.
Each parotid gland sits on either side of the face. They excrete saliva into the parotid ducts, which carry the saliva into the mouth. The ducts empty into the upper jaw, which allows the saliva to cascade over the teeth and amply lubricate the mouth. In addition to the parotid glands, two submandibular glands secrete saliva into the lower part of the mouth. Because all of these glands use ducts to deposit their secretions, they are considered exocrine glands. This is opposed to endocrine glands, which secrete hormones directly into the bloodstream or extracellular space.
Parotid Gland Function
When we are at rest, or not eating, the parotid glands account for about ten percent of the saliva in our mouth. It is essential to keep our mouth lubricated at all times to protect the delicate linings of our alimentary canal as dryness can lead to broken skin through which pathogens can enter. However, once activated they will secrete upwards of twenty-five percent of the saliva in our mouths. This increase is imparted by the body’s need for amylase to start the digestion of starches. The main function of parotid glands, like salivary glands in general, lies in facilitating the digestion of food. How is this done? By secreting saliva!
Mastication, or chewing, is the action that precedes the release of saliva from the salivary glands. Aside from our teeth physically breaking down food, the first step of digestion requires the molecular breakdown of the complex carbohydrates as well. Our gut will need simpler sugars to properly absorb nutrients from our food, so the gentle digestion of starches will begin at the point of entry – the mouth. There are various cell types within the gland that allow saliva secretion. For example, acinar cells are berry-lobed cells that will expel enzymes.
Though salivary glands are always working – especially the parotids as they are the largest and biggest producers of saliva – they are prone to infections and are even affected by our water intake.
Parotid Gland Location
The parotid gland is located under the skin, between several muscles, just in front of each ear. The gland can be felt when it is swollen or inflamed, which is typically why doctors feel this area of your cheek during a checkup. The ducts of the parotid lie adjacent to the top row of teeth, helping ensure the entire gut stays well lubricated. Further, the large masseter muscle of the jaw sits just below the parotid, helping move the saliva secretions into the mouth when chewing.
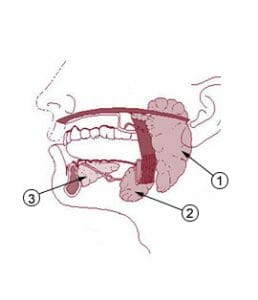
The figure depicts salivary glands, the left parotid gland is labeled number one.
If we were to visualize the location of the glands, they lie in front of and beneath the ears. The word parotid, in fact, is a literal translation for “beside the ear.” Likewise, the parotid gland can be thought to wrap around the lower jaw bone or mandible. It appears in the shape of a wedge and can be felt on either side by running our fingers from in front of the ear down the cheek. Each parotid gland channels saliva through the parotid duct. The parotid duct is a long tube that exits in front of the parotid glands and is superficial to (closer to the skin compared to) the jaw’s masseter muscles.
Parotid Gland Development
Parotid glands begin to form at around the sixth week of gestation. They are the first salivary gland to form. They start off as little epithelial buds near the lips of the primitive mouth. These buds will move toward the back, closer to the otic placodes of the ears. The ducts that channel through the parotid glands will form at the tenth week. The ends of the ducts will become populated with the secretory acini cells, which only eighteen weeks into gestation will begin to secrete into the parotic duct!
As the parotid gland takes mature form, it will receive innervation from the parotid plexus, or branches of the facial nerve bundle. Parasympathetic innervation by the glossopharyngeal nerve will make us salivate. Meanwhile, the trigeminal nerve will give it sensation. The external carotid artery will be the major supply of blood for the parotid gland, and drainage will be made possible by the retromandibular vein.
Parotid Gland Infection
Parotid glands have the largest surface area, and so there is physically more area for infection. Infection often begins with blockage of the salivary ducts by stones. Salivary stones are calcified masses that form on the inside of a duct. They are more common in submandibular glands, but sometimes the parotid gland will also experience this blockage. This will block the normal flow of saliva through the ducts, which will result in swelling and inflammation.
Infection by bacteria or viruses can stop salivary ducts from functioning normally. For example, the mumps virus will cause the parotid glands to swell with inflammation called parotitis. Those affected will experience tremendous pain. A common way that this illness is detected in the doctor’s office is by testing the blood for high levels of salivary amylase since the parotid glands will work overtime to secrete it.
So how are these blockages removed? Well, salivary stones can be removed by surgically opening the site of the blockage. This works particularly well for stones that are located more superficially. However, if the stone is deep in the duct the gland may need to be excised completely. For parotitis, a combination of massage, irrigation, and antibiotics may be in place. In other cases, surgical ligation of the duct may be required to prevent further injury.
Parotid Gland Tumor
Resection of parotid gland tumors is a little more complicated. Of all salivary gland tumors, seven out of ten start in the large parotid glands. About eight of ten parotid tumors will be benign. The salivary mass can be aspirated away with a biopsy. But very rarely, a cancerous tumor emerges. Malignant tumors will be rock hard, and will often include fixed skin or skin ulcers. Many of the cancers are a type of adenocarcinoma, which describes cancers that start at secretory gland cells.
Treatment for malignant parotid tumors is normally excision and radiation treatment. Radiation will effectively target and destroy cancer cells in the parotid gland. Malignant salivary gland cancers normally come in three grades:
- Grade 1 cancer: low grade. The salivary gland cells look quite normal, and they grow slowly so they have a better chance of a good prognosis
- Grade 2 cancer: intermediate grade. Their appearance and prospects are middle of the road between grade 1 and 3 cancers
- Grade 3 cancer: high grade. The salivary gland cells look very different from normal and will spread rapidly. The outlook is normally lesser than lower grade cancers.
Quiz
