Definition
A sperm cell or spermatozoon is a gamete (sex cell) produced in the male reproductive tract. It is a motile cell with a single aim – to fertilize a female egg. Each sperm cell contains the entire genome of the male that produces it. In combination with the female genome contained within the egg, a zygote is formed – a single totipotent stem cell containing the fused genome of both male and female. Sperm cells (spermatozoa) were first described in the late seventeenth century by Antonie van Leeuwenhoek.
Sperm Cell Structure
A sperm cell is one of the smallest cells of an organism and is produced by most animals and some plants. Spermatozoa are divided into motile and non-motile groups. The non-motile sperm cell (spermatium) is produced by some algae, fungi, and lichen species. Motile sperm cells are produced by animals and some plants; some plant sperm cells have more than one flagellum. The sperm cell diagram below shows multiflagellate fern cells.
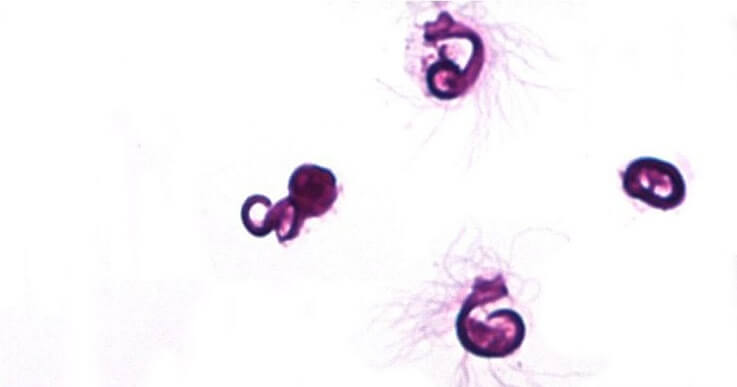
Most motile spermatozoa have flagella to help them swim through fluids – the seminal fluid produced by males and the mucus membranes of the female reproductive tract. Flagellum movement requires a consistent energy source.
Sperm cell adaptations include a low-friction, tapered shape, a large energy-producing component, alkaline characteristics that counteract the acidic environment of the female reproductive organs, and a chemical sensor that can locate the egg.
In mammals, a sperm cell is composed of a head, body, and tail (flagellum). A sperm cell under microscope lense is instantly recognizable. How many chromosomes in a sperm cell? A human sperm cell contains half of the number of chromosomes found in non-sex cells that contain a nucleus – twenty-three. The chromosomes in spermatozoa are not paired – a sperm cell is, therefore, a haploid cell.
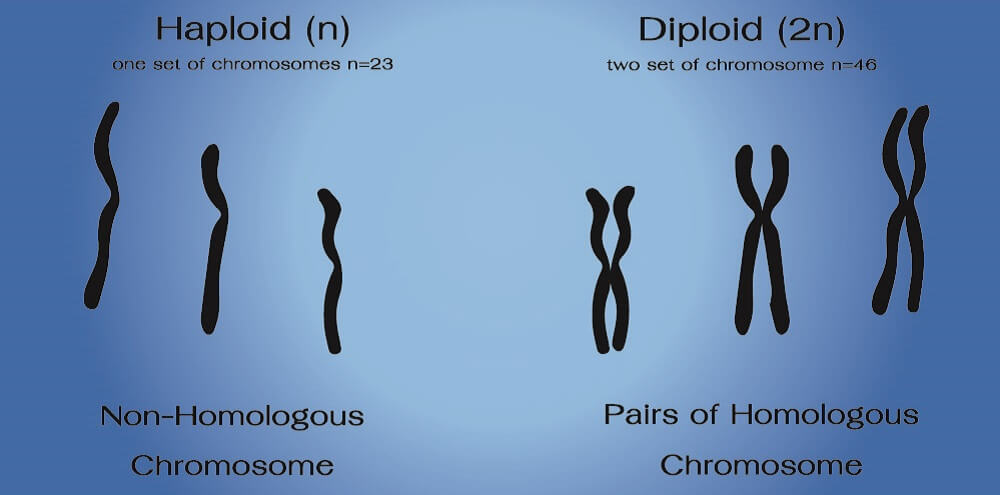
Only gametes – the egg cell and sperm cell – have a single set of twenty-three chromosomes. When they fuse to produce a zygote, that cell contains twenty-three chromosome pairs; a mix of the genetic information of the male and female. The zygote is a diploid cell, as are the rest of our nucleated non-sex cells (somatic cells).
Sperm Cell Head
The average spermatozoon has a smooth, nearly oval head that measures between 2.5 and 3.5 micrometers in width and 4 to 5.5 micrometers in length. Beginning at its center, the spermatozoon head is composed of:
- Nucleus
- Small amount of cytoplasm with nuclear vacuoles
- Nuclear membrane
- Inner acrosomal membrane
- Subacrosomal space
- Acrosome and acrosomal cap or post-acrosomal region
- Outer acrosomal membrane
- Peri-acrosomal space
- Plasma membrane
Scientists have not yet agreed upon the origin and function of nuclear vacuoles, but it seems that the more vacuoles are present, the less fertile the sperm.
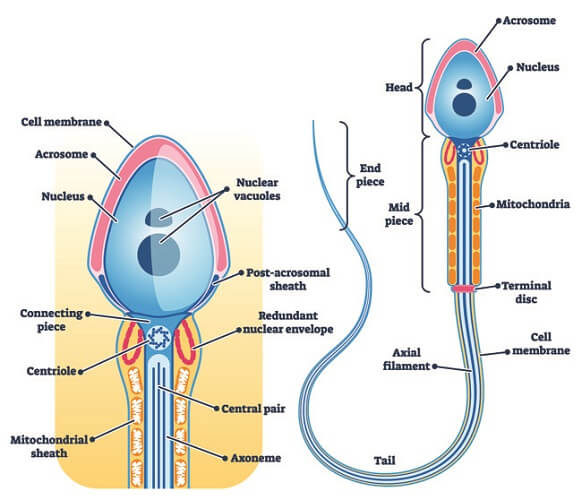
The acrosome does not envelop the entire head and its coverage varies per cell. This organelle develops from the Golgi apparatus of an immature sperm cell and contains hydrolytic enzymes and polysaccharides. The sugars provide the cell with energy; the enzymes allow the sperm cell to move through the cumulus cell layer and zona pellucida of an egg, enabling fertilization. A sperm cell without an acrosome is infertile.
When the acrosome first comes into contact with the cumulus, it sets off a process called the acrosome reaction; stored enzymes are released when the acrosome breaks down during the successful cell’s journey deeper into the egg.
Another acrosome function is to locate the released egg by way of chemotaxis. This organelle can sense tiny concentrations of progesterone secreted by cumulus cells; however, the exact mechanism is not yet understood.
A plasma membrane covers the entire spermatozoon; recent research reports the presence of lipid rafts (lipid ordered microdomains). Lipid rafts seem to play important roles in cell signaling and membrane trafficking (moving proteins and other large molecules through a cell membrane). The sperm cell lipid raft probably contributes to the acrosome reaction.

Sperm Cell Body
Each sperm cell body, sometimes referred to as the midpiece, contains fifty to seventy-five mitochondria – energy-producing organelles – and two centrioles.
Mammalian spermatozoa have one conical and one atypical centriole, both of which are necessary for sperm cell spermatogenesis in the testes (see next heading). Once a mature sperm cell has formed, these centrioles have additional roles – they fuse the head to the tail and control tail movement. Finally, when the sperm cell fertilizes an egg cell, the centrioles help form the resulting zygote’s cytoskeleton.
Sperm cell bioenergetics describes how a spermatozoon produces sufficient energy to move through approximately four inches of mucus. While four inches does not seem so far, this is the equivalent of a human going for a thirty-mile swim. As a healthy spermatozoon can cover four times its body length in one second, this is the equivalent of a human swimming thirty miles in less than two hours. With a typically zig-zag route, this matches the distance of an English Channel swim, of which the fastest speed ever recorded was slightly under seven hours.
Mitochondria convert sugar into the energy they need and send most of this energy to the flagellum. Sugar is provided by seminal fluid as well as the mucus membranes of the female reproductive tract.
Sperm Cell Tail
The majority of a sperm cell’s length is composed of its flagellum. The tail has a principal piece and an end piece; both parts are essential for sperm cell motility. Central is the axial filament or axoneme formed by the atypical centriole during spermatogenesis.
A spermatozoon moves in two different ways: activated and hyperactivated. Hyperactivated mode occurs when a sperm cell makes contact with an egg or becomes trapped. We now know that sperm cell flagellum movement is not whip-like as formerly proposed. By slowing down sperm cell motility on a 55,000 frames-per-second, three-dimensional microscopy set-up, scientists have shown that the tail only beats in a single direction in combination with sperm cell head rotation. This is similar to the movement of a drill bit.

Spermatogenesis
Spermatogenesis occurs in the testes. It takes about two months to produce spermatozoa from a germ cell and consists of three phases:
- Spermacytogensis: a spermatogonium or unipotent germline stem cell (GSC) is an undifferentiated cell that can only differentiate into one other cell type. This cell remains silent (G0 of the cell cycle) until puberty, although spermatogenesis begins shortly after birth with the production of spermatogonia. Either a GSC produces more of its own type to ensure continued production of spermatozoa, or it divides to produce two primary spermatocytes. Both the original stem cell and its partially differentiated spermatocyte daughter cells are diploid cells – they contain twenty-three chromosome pairs in their nuclei (forty-six chromosomes, as with any somatic cell). The next round of cell division divides the primary spermatocytes into secondary ones, and shares the chromosomes rather than replicating them. Each secondary spermatocyte is haploid and contains twenty-three chromosomes, not twenty-three chromosome pairs.
- Spermatidogenesis: when the two secondary spermatocytes divide they produce four haploid spermatids.
- Spermiogenesis: under the influence of the hormone testosterone, the spermatids grow tails (originating from the centrioles). Their inactive DNA (that does not produce proteins) is condensed into chromatin. The Golgi apparatus changes its form and becomes the acrosome; the cytoplasm shrinks. Less essential organelles disintegrate and may be the source of nuclear vacuoles. Once spermiogenesis has taken place, spermatids are called spermatozoa. These are mature cells capable of fertilizing a female egg.

Sperm Cell Function
Sperm cell function is singular – to fertilize a female egg and produce the next generation of a species, so passing on the male’s genome. This single function is made clear in the third phase of spermatogenesis where all unnecessary organelles disintegrate. The sperm cell is, very simply put, DNA with an engine.
A spermatozoon produces energy when nutrients are freely available. This energy drives movement through the female reproductive tract, giving it a greater chance of fertilizing the egg.
Spermatozoa are constituents of sperm. The other component of sperm is seminal fluid or semen. Semen is a high-fructose fluid produced primarily in the seminal vesicles and prostate gland. As well as sugar, it contains amino acids, citrate, zinc (a DNA-stabilizing element), salts, and prostaglandins. Prostaglandins lower the risk of a female immune system response to the spermatozoa.
A healthy human male produces approximately 1,500 spermatozoa per second. One milliliter of semen contains anywhere between twenty to three hundred million sperm cells. Each ejaculation produces two to five milliliters of semen.
Sperm Cell Infertility
Infertility is the inability to conceive naturally within the first year of unprotected sexual intercourse without use of birth control medication. Extremely low sperm counts account for around 15% of males who are unable to reproduce without medical assistance.
The World Health Organization reports that up to 80 million people suffer from this problem; less than half of these cases are purely due to male infertility. Although many causes lead to the inability of a male to reproduce, more often than not the reason is unknown. Current knowledge of spermatogenesis and the mechanisms of the acrosome is extremely limited.
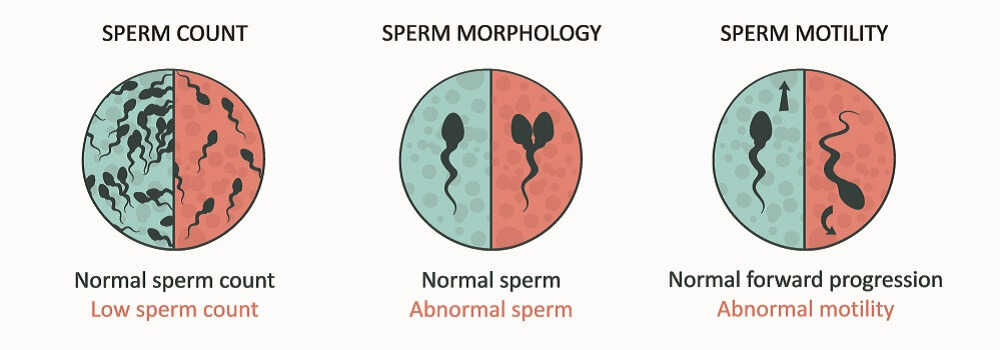
The primary known causes of male infertility that affect sperm cell quality and function are:
- Hormonal imbalances: the male hypothalamic-pituitary-gonadal axis regulates testosterone, luteinizing hormone, prolactin, and follicular stimulating hormone. Imbalance in any one of these hormones can affect fertility levels.
- Genetic factors: chromosomal abnormalities present from birth can interfere with spermatogenesis; this problem can only be expected to worsen. Modern fertility techniques (assisted reproductive techniques) have made it possible for many infertile males to reproduce; when sons are born to men with genetic causes of infertility, these genes can be passed on through the Y chromosome.
- Epigenetic factors: faulty gene expression can affect early spermatogenesis. It has also been shown to lower sperm cell capacitation – the ability of a spermatozoon to penetrate and fertilize an egg. Molecular elements include a range of single nucleotide polymorphisms (SNPs) or ‘snips’ (genetic variations of the nucleotides of our DNA) that inhibit spermatozoa production, maturation, and capacitation to varying degrees. Genome-wide association studies are looking at the combinations of faulty gene sequences that cause male infertility.
- Environmental factors: exposure to pesticides, solvents, and radiation has been shown to affect the shape of sperm and so reduce sperm cell motility. Chemotherapy for male cancer patients also has a negative effect on spermatozoa quality.
- Physical disorders: urinary tract infections, mumps, and sexually transmitted diseases are just a few examples of physical disorders that can lead to testicular atrophy or male reproductive tract obstruction. While an obstruction may not affect sperm cell health, testicular atrophy can. Hyperglycemia in male diabetes patients disrupts the spermatogenetic process, although the exact mechanism is not yet understood.

Most FDA-approved male infertility drugs work to regulate hormone levels. Diets high in antioxidants reduce the levels of reactive oxygen species (ROS) in seminal fluid; ROS are associated with sperm cell dysfunction and, in some men, a diet high in vitamin C has improved fertility. The future may look at induced pluripotent stem cells (iPSCs) that can be genetically engineered to produce spermatazoa and are then transplanted into the testes.

