Lesion Definition
A lesion is an area of inflammation in a tissue that suffered trauma or the impact of chronic illness. Typically, a lesion involves an abnormal structural change to a tissue. So, it is often defined as a site of abnormal tissue change. These changes can take place in the form of wounds or bruising, but is also a term used by oncologists to describe wounds caused by malignant or benign (innocuous) cancers.
Lesions, of course, vary in severity depending on their size and location. While some are completely harmless, others are serious or even life threatening. Luckily, inspection during a doctor’s visit can identify a lesion and predict its harmful impact. Tools clinicians have at their disposal for diagnosis are x rays, biopsies, MRI, blood analysis tests, and neurologic or physical exams. These latter exams are important in evaluating the effect the lesion has had on the patient’s reflexes, coordination, balance, vision, and language centers. A lesion can certainly compromise these abilities given that the body is wired so that any severed connection can have a lasting impact on coordinated processes like movement or hormone production (if an organ or gland is severed).
Lesions can be classified by the visual patterns they create. An x ray scan of the gastrointestinal tract, for instance, can reveal ulcer craters. The sickle cell “s” shape of red blood cells with anemia is an example of a molecular lesion that can be seen histologically. Likewise, a tumor can present an either target or bull’s-eye pattern. Lesions left behind by illness, like the Ghon lesion scar in the lungs of adults with childhood tuberculosis, is another example of the insight that lesion analysis can give.
Lesion Examples
Lesions can arise in varied places and for varied reasons ranging from the impact of an injury to a viral infection. Below we will discuss a few groups of commonly acquired lesions.
Skin Lesions
While lesions can occur on any site inside our bodies, one of the more visible places to incur lesions is on our skin. Skin lesions are patches of skin that have undergone abnormal structural changes. They can be separated into either primary or secondary groups. Primary lesions refer to those that vary in color or texture and may have been present at birth. These lesions are quite common since our epidermis has a large surface area, and therefore has the potential to acquire many types of lesions over the course of our lifetimes. Blisters, for example, are commonly attained and can arise from sun exposure or friction against our skin. Acne sufferers will be familiar with papules and pustules, which are really small skin lesions filled with pus. Cysts are similar pockets of pus but are buried deeper in the skin. Freckles and flat moles are examples of macule skin lesions. Nodules refer to “knot” like growths of abnormal tissue that develop under the skin. For instance, lymph nodes can develop nodules that are visible from the surface of the skin upon inspection. Skin tags and moles are also common skin growths that often call into question whether they should be left alone, or removed if malign.
Secondary skin lesions are a bit more nuanced. Some examples of secondary lesions include ulcers, which perforate the epidermis such that the dermis layer is exposed. The scales or dead skin flakes that form from psoriasis or dermatitis are another example. Scabs and scars that form in the healing (and post-healing) stages after an injury are also classified as secondary tissue lesions. Erosion occurs when the surface-most dermal layers are lost, and excoriation creates a hollow area from picking at a primary lesion. The underlying factors that give rise to skin lesions vary. Eczema or birth marks are inherited at birth. Scarring and scabs result after incurring skin infections by viruses, bacteria or fungi, or even acne – which affects not only teens but adults, also.
Detecting these outer skin lesions is helpful in identifying (and treating) skin disease. But perhaps one of the best detection guidelines in examining moles and skin irregularities lie in the ABCs of skin cancer:
- Asymmetry: an abnormal mole will not be round or even
- Border: an abnormal mole will not have a defined or regular border
- Color: an abnormal mole will likely not be uniformly tan but instead a mixture of colors.
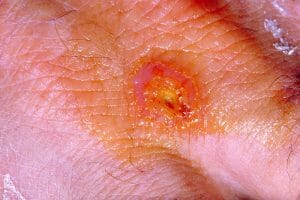
Pictured is a tularemia skin lesion on a patient’s right hand, caused by a bacterium Francisella tularensis that causes skin ulcers
Brain Lesions
Brain lesions are a site of injury to the brain. Understanding cerebral lesions is quite complex, since any severed connection can have permanent consequences on personality or thinking and action processes. Brain lesions come in different sizes and can be varied in number. Depending on these factors, they can be determined to be harmless or a threat to life. There are numerous ways of acquiring a brain lesion, such as injury, immune problems, or infection, but the truth is many are acquired by unknown means. Similarly, brain lesions may vary by size, location, and type.
Brain abscesses, or cysts, are sites of inflamed tissue that develop puss. They are rare, but life threatening. They are known to appear after a nearby infection (i.e. ear infection) but also from a blow to the skull. Cerebral infarctions (or “strokes”) are another type of lesion caused by a cluster of cell dying as a result of not receiving adequate blood. Arteriovenous malformations, or AVMs, are tangled knots of arteries and veins that prevent brain tissue from getting a healthy supply of blood. Multiple sclerosis is another disease that is auto immune and severs the myelin that coat nerves in the brain and spinal cord. These lesions muddle the information sent between the brain and the body. In infants, cerebral palsy emerges from brain lesions received in the womb. Brain tumors, likewise, can lead to blockage or worse, metastasize into cancer. Removal may involve surgical resection, but also chemotherapy or radiation therapy for cancerous lesions.
Common clinical signs of a brain lesion include:
- Nausea
- Vision changes
- Memory loss
- Seizures
- Mood changes
Inner Organ Lesions
As previously alluded to, our inner organs are also subject to lesions that often require surgical resection. Liver lesions, for instance, may either be asymptomatic or symptomatic. Benign (or harmless) masses of cells form in the liver and are either solid, or cysts (with fluid). Of the most common solid masses to form, hemangiomas are the most common and are lesions of less than 6 cm that form from compression injuries. The most common liver cyst forms in the bile duct and causes vomiting, jaundice, and right rib cage pain. In lungs, a single pulmonary nodule (SPN) growth can form. It is typically asymptomatic but can be spotted by a chest x ray or CT scan, followed by a biopsy to test if the nodule is cancerous or benign. Lesions in the spinal cord also form, secondary to trauma or infections like HIV. These can result in motor or sensory issues, if not worse in death.
Quiz
1. Define primary skin lesions:
A. They are raised sections of skin
B. They vary in size and texture
C. They are embedded deep, under the epidermis
D. They vary in color and texture
2. Correctly name what the ABCs of skin lesions stand for:
A. Abnormality, base, color
B. Asymmetry, border, color
C. Asymmetry, base, color
D. Application, border, color
References
- Web MD (2017). “Brain Lesions: Causes, Symptoms, Treatments.” Web MD: Brain & Nervous System. Retrieved on 2017-06-09 from http://www.webmd.com/brain/brain-lesions-causes-symptoms-treatments#1
- Page, Elizabeth MD (2017). “Diagnostic Tests for Skin Disorders.” Merck Manuals. Retrieved on 2017-06-10 from http://www.merckmanuals.com/professional/dermatologic-disorders/approach-to-the-dermatologic-patient/diagnostic-tests-for-skin-disorders
- National Multiple Sclerosis Society (2017). “Diagnosing Tools.” NMS. Retrieved on 2017-06-09 from http://www.nationalmssociety.org/Symptoms-Diagnosis/Diagnosing-Tools
- Medical Dictionary (2017). “Skin Lesions.” The Free Dictionary. Retrieved on 2017-06-08 from http://medical-dictionary.thefreedictionary.com/Skin+Lesions
- Sutter Health CPMC (2017). “Non-Cancerous Liver Lesions Diagnosis and Treatment.” CPMC. Retrieved on 2017-06-08 from http://www.cpmc.org/advanced/liver/patients/topics/noncancerous-lesions-profile.html
