Corpus Luteum Definition
The elusive corpus luteum is a temporary structure with crucial roles in ovulation and the beginning stages of pregnancy in women. The corpus luteum forms after a follicle has released an egg during ovulation. The hormones secreted, mainly progesterone, ready the body for pregnancy.
Corpus Luteum Overview
Upon closer look, the corpus luteum is a yellow-tinged mass that lies atop the female ovaries. It begins to form at the site of the follicle after it has matured and is commencing the process of ovulation. Ovulation, in turn, describes the process by which a mature follicle is finally able to rupture and release an egg that can be fertilized by a sperm cell. This rupture, then, is what makes pregnancy possible – thus revealing the important role that the corpus luteum holds in sustaining life.
The corpus luteum is formed in the ovary and is made up of a cell type called the lutein cell. Lutein cells are granulous cells with a pale cytoplasm that is rich in lipids that will begin to develop and build up fatty lipids and yellow pigment within the lining of the follicle. This lends the tissue a yellow appearance. The corpus luteum is thought of as a temporary endocrine structure.
The reason for this is that while this tissue begins to form soon after the ovum is released through the fallopian tubes, it will start to break down merely a few days after it forms unless a fertilization event has occurred. Moreover, the corpus luteum is capable of releasing hormones, like all endocrine organs. The principal hormone released is the very well-known female hormone, progesterone. This hormone has roles in the development of the endometrium and its upkeep.
Corpus Luteum Function
The corpus luteum’s main function can be distilled down to its role in supporting the early pregnancy in the female body. It does so by releasing progesterone and estrogen. This mixture will cause the uterine mucosa to undergo all of the changes it needs to prepare for the successful implantation of a fertilized embryo. Progesterone is mostly released in the latter half of the menstrual cycle in a timeline that matches the structural changes occurring in the ovaries.
During the Menstrual Cycle
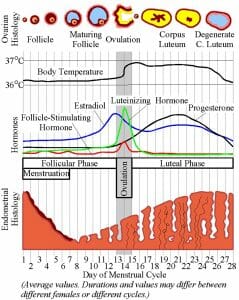
If the menstrual cycle is mapped out along with the levels of female hormones circulating the body, certain relationships are revealed. The early stages of follicle formation in ovarian histology is called the follicular phase and occurs in the first 12 days of the menstrual cycle. The follicular phase will coincide with a steady rise in the follicle-stimulating hormone (FSH) and estradiol that promote the maturation of the follicle. Around the 13-15th day of the menstrual cycle, however, the ovaries will experience ovulation and rupture, and there will be a notable spike in the FSH and luteinizing hormone (LH) circulating the body.
However, ovulation is short-lived and will end on the fifteenth day of the menstrual cycle as the corpus luteum begins to form. This appearance in the so-called luteal phase will follow a decrease in FSH and LH hormones in favor of a rise in progesterone hormone. The luteal phase will continue until the corpus luteum disintegrates and the menstrual cycle commences again if a fertilization event has failed to occur. In effect, there is a real link between the morphological changes occurring in the ovary and the female hormones that are released.
The figure graphically depicts the correlative timelines of ovarian histology, hormone release, and endometrial histology over the course of the female menstrual cycle.
Corpus Luteum After Fertilization
In the event that pregnancy does occur, it will be important to prevent the disintegration or shedding of the corpus luteum that normally occurs with menstruation. In order to preserve the hormone-secreting tissue for the delicate embryo to survive, the trophoblast of the embryo will combat the regular drop in progesterone by producing human chorionic gonadotropin, which is very similar to LH. This will allow the survival of the corpus luteum as it enlarges during pregnancy until the placenta is able to make enough progesterone and estrogen to maintain the uterus’ mucosa. The levels of progesterone will continue to rise throughout pregnancy to ensure the proper development of the fetus and the mother’s pelvic walls.
Furthermore, estrogen or progesterone released by the corpus luteum is said to directly inhibit the release of follicle stimulating hormone, thus explaining its sharp decline at the time when the corpus luteum begins to forms. This has an evolutionary purpose of preventing the creation, and later maturation, of a follicle. This, of course, prevents a double pregnancy. Without this inhibitory step, multiple ovulations could occur.
Corpus Luteum Disorders
While the corpus luteum is a temporary structure, it can sometimes grow too large, forming a corpus luteum cyst. These cysts are usually not deadly, though they do cause pain. Typically, the cysts will go away within a few days to a week. However, a large corpus luteum cyst can become hemorrhagic, meaning it causes internal bleeding and increased pain. In the worst cases, the cyst can become so large it causes the ovary to twist. This condition, called ovarian torsion, is extremely painful and may need surgical intervention.
Quiz