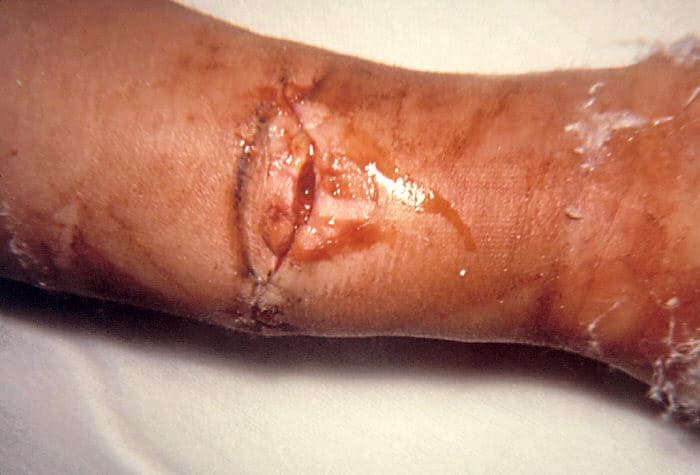
Definition
Clostridium botulinum is a species of the Clostridium genus that produces and secretes the powerful neurotoxin called botulinum toxin. C. botulinum bacteria are anaerobic, gram-positive bacilli found primarily in food items, freshwater sources, and the soil. While the poisoning known as botulism used to be fatal in up to 60% of cases in the 1950s, mortality has now been reduced to below 3%.
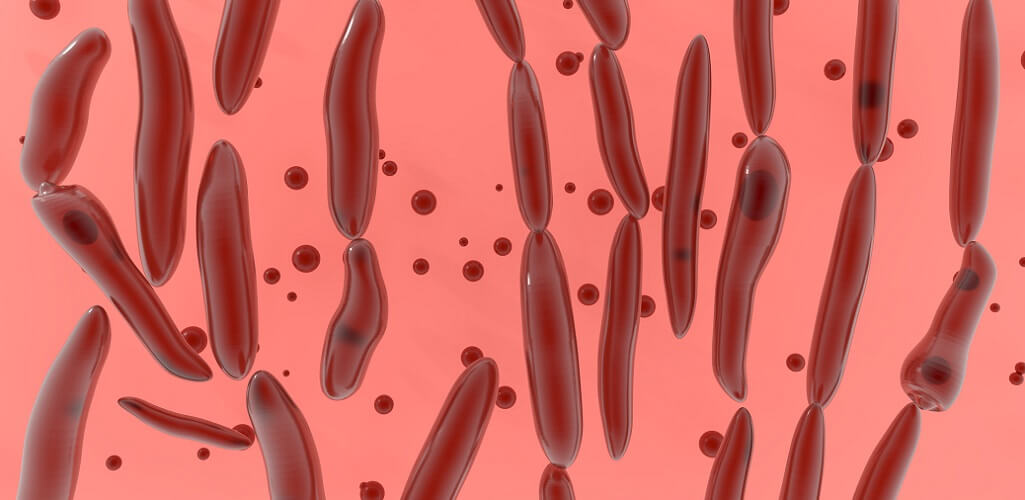
Clostridium Botulinum Bacteria
Clostridium botulinum bacteria thrive in low-oxygen environments. They are rod-shaped bacilli that form spores when conditions are less than ideal. Acidity levels under 4.6 pH stop Clostridium population growth.
Clostridium botulinum secretes botulinum neurotoxins or BoNTs of varying serotypes. The most deadly of these is botulinum toxin type E. This is the most deadly toxin known to man.
We now know much more about Clostridium botulinum thanks to whole-genome sequencing. This science has led us to divide Clostridium bacteria into two human groups – proteolytic C. botulinum (Group I) and non-proteolytic C. botulinum (Group II). A further two groups describe non-human forms. Group III is associated with the presence of botulinum toxin in animals, and Group IV with toxin production neither in humans nor animals.

Proteolysis refers to the toxin’s ability to break down certain proteins or amino acid chains. Botulinum toxin specifically attacks glycoproteins in cholinergic nerve endings.
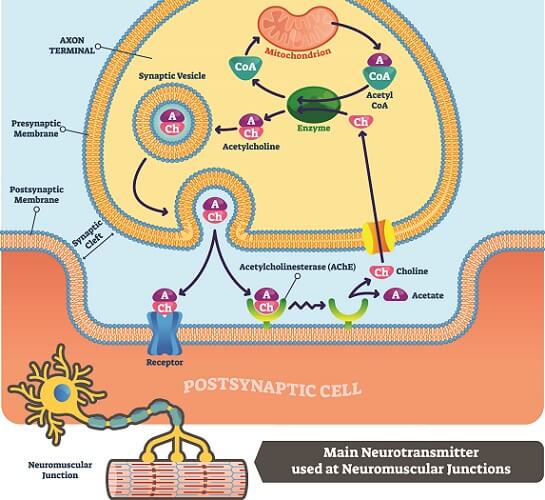
These glycoproteins form membranes that fuse to release neurotransmitters from the nerve terminal. The neurotransmitter can then cross the nerve synapse to the next nerve cell or target cell.
Proteolytic toxins break down the proteins of some of these glycoproteins. Non-proteolytic toxins act upon the carbohydrate part (glucose or maltose, for example) of the glycoprotein.
Both types of action stop the transmission of the neurotransmitter acetylcholine.
Clostridium botulinum in Group I grow in temperatures between 12°C and 37°C; the optimal growth temperature is 37°C – mammalian body temperature. Outside of these temperatures, Group I C. botulinum forms spores. These spores are particularly good at surviving very high temperatures. Strains of Group I bacteria can form three types of neurotoxin (A, B, or F).
Group II is a psychrotroph – a cold-tolerant bacteria that can grow at low temperatures, although the best growth conditions are around 20°C. Group II Clostridium botulinum will grow at 3°C and continue to multiply at temperatures of up to 30°C. Group II spores are not as heat resistant as Group I. Group II secretes serotypes B, E, and F of the botulinum neurotoxin.

Group III Clostridium botulinum is responsible for avian or nonhuman botulism outbreaks in wild and domestic animals, especially herbivores like cattle, horses, and sheep. Poultry and waterfowl are also susceptible. The genetic makeup of this bacterial group is very different from Groups I and II. These bacteria produce different botulinum toxin serotypes (C or D) and are non-proteolytic.
Group IV C. botulinum is rare. It produces type G botulinum toxin that is proteolytic. While it had formerly not been identified in humans or animals but as a soil-based bacteria, a famous report listing five unexpected sudden deaths due to the presence of type G toxin shows that this group may eventually be categorized as a human serotype.
Clostridium Botulinum Toxin
Clostridium botulinum toxin is listed as a Category A bioterrorism agent on the Centers for Disease Control and Prevention website. This is the highest risk category and lists the bacteria and viruses that cause anthrax, botulism, plague, smallpox, hemorrhagic fevers, and tularemia.

All of these diseases are highly contagious and can be fatal, especially without treatment or if large populations become infected within a short period, leading to low levels of the drugs that treat these conditions.
In World War II, US soldiers were immunized with an antitoxin before arriving in France due to fears of the German army using Clostridium botulinum as a biological weapon. Iraq admitted to producing 19,000 liters of concentrated botulinum neurotoxin in the 1990s, and even small terrorism groups have been able to grow botulinum from spores found in the soil. So far, a method in which to spread this toxin throughout large areas has not been found.
Clostridium botulinum toxin has many therapeutic uses. As it stops muscles from contracting, pathologies such as painful muscle spasms, chronic eye twitches, some types of urinary incontinence, and torticollis (or wry-neck) can be effectively treated with botulinum toxin injections.

While most professionals associate botulinum toxin with motor neurons, it also affects sensory nerves. A small amount can even cross the blood-brain barrier. Because of this, Botox can be used to alleviate chronic neurological pain.
We usually associate Botox injections with cosmetic procedures that slow the signs of aging; muscles that are directly attached to the skin can cause facial lines. When these muscles are forced to relax, these lines fade. The average Botox injection lasts for around three months.
Clostridium Botulinum and Botulism
When a person or animal is infected by C. botulinum, they may contract clostridium botulism. The main source of infection is food. Clostridium botulism is not transmitted between animal to human or human to human unless contaminated fecal matter enters the digestive tract or wounds.

The average adult only needs to ingest 60 to 80 nanograms of botulinum toxin to die from the effects. If this is absorbed via other ways, such as in a nose-spray, aerosol or injection, less than 10% of the oral dose can cause death.
How ill a person or animal becomes depends on how concentrated the toxin is and how many bacteria or bacterial spores enter the body; the higher the dose, the more rapid the effect. It should be made clear that Botox is not the injection of C. botulinum bacteria but of the toxin these bacteria produce. The toxin will not replicate inside the body.
A clostridium botulism infection has certain characteristics in humans and animals. The mean incubation period of mammalian bacteria types is most commonly one to three days, sometimes as much as ten days.
Initial Clostridium botulinum symptoms are vomiting and diarrhea in early stages and constipation later on. Various forms of muscle paralysis can occur:
- Ciliary muscles: blurred or double vision and dilated pupils (mydriasis)
- Facial muscles: dry mouth, slurred speech, drooping eyelids, difficulty swallowing
- Skeletal muscles: limb weakness or paralysis
- Respiratory muscles: breathing difficulties
Breathing difficulties occur in untreated botulism and may be fatal.
There are three clinical forms of botulism – foodborne, infant, and wound.
Foodborne Clostridium Botulism
Foodborne clostridium botulism used to be a very common infection. The severity of symptoms depends on the type of neurotoxin (A, B, or E), and the amount of neurotoxin produced and absorbed.
Packaged foods that do not contain high levels of acids are most likely to contain C. botulinum bacteria or their spores. Remember that Group I spores can survive very high temperatures. Home canning is a prime source when the ingredients or low-acid canning liquids are contaminated before sealing.

Botulism is named after the main source of infection in the eighteenth century – sausages. The Latin for sausage is botulus.
The advent of canned food is in the late eighteenth century after Napoleon Bonaparte offered a twelve thousand franc prize to the person who developed a reliable method of food preservation. Popularity grew and this proved an easy way to ensure Civil War soldiers got their rations. As an anaerobic bacteria, the inside of a can provides perfect conditions for Clostridium botulinum.

Between the end of 1919 and the start of 1920, eighteen people died in the USA after eating canned black olives from California. This lead to the funding of a Botulism Commission and today’s strict processing regulations. In 1931, twelve adults and children died at a dinner party in North Dakota. And in 1977, the largest recorded outbreak occurred at a Michigan restaurant where nearly sixty people became ill after trying the homemade salsa. Food Codes now prevent foodborne botulism in most countries.
Clostridium botulinum prevention in food sources regulates safety measures for preparation and packaging. Nitrates or nitrites are added to cured meat, preparation areas must be sterile, and canned foods are heated at temperatures of 250°F (121°C) under steam pressure for a period dependent upon the foods’ acid content. Adding salt to water to produce brine also prevents Clostridium botulinum growth; restricting water levels in low-oxygen packaging is also essential.

Reduced-oxygen packaged foods should be refrigerated at temperatures under 38°F or 3.3°C. These foods, when reheated, should be thoroughly cooked at high enough temperatures. For more information about finding C. botulinum colonies in food samples, read this Food and Drug Administration Bacteriological Analytical Manual page.
Infant Botulism
Children under a year of age do not have functional gut microbiota and are more likely to pick up and incubate C. botulinum bacteria in the intestine. Intestinal toxemia botulism is primarily of the infant type but can be seen in adults with digestive tract pathology or in those treated with antibiotics.

A child that ingests as few as ten Clostridium botulinum spores can develop botulism. Spores can be dust-borne or present in food. Honey is highly associated with infant botulism transmission; this cause is so prevalent that the CDC website specifically advises that children younger than twelve months of age should not be given honey.
Even babies under a month of age can contract infant botulism. Very few cases lead to death after Clostridium botulinum treatment with intravenous botulism immune globulin (BIG-IV). BIG-IV is a purified immunoglobulin (antibody) produced by adults who have been immunized with botulinum toxoid types A and B.

Botulinum vaccines are a form of passive immunization. Immunoglobulins bind with unbound botulinum neurotoxin molecules. This stops unbound toxins from blocking the release of acetylcholine at the nerve synapse but does not remove those that have already bound the previously-mentioned glycoproteins. Because of this, BIG-IV should be given as early as possible as it will not reverse existing symptoms. It does, however, prevent symptoms from becoming worse.
Wound Botulism
Luckily, wound botulism is very rare. Most people who contract wound botulism are intravenous drug users. As cases are usually found in clusters, it is probable that the drug itself is contaminated and not the needles or other equipment. In January 2015, the British Broadcasting Corporation (BBC) released a series of reports about several Scottish heroin users that had all been admitted to hospital with botulism poisoning within a few short weeks.
Very few cases of wound botulism have been reported as the result of open traumatic wounds, such as has occurred in this open fracture.