Definition
Alanine aminotransferase (ALT) is an enzyme produced primarily in liver and kidney cells but also found in smaller quantities in the muscles and heart. When the liver is damaged, blood alanine aminotransferase levels rise. ALT is important as it can convert the amino acid alanine into pyruvate. Pyruvate is part of the Krebs cycle that produces cellular energy. A blood serum alanine aminotransferase test is used to detect liver damage.
What is Alanine Aminotransferase?
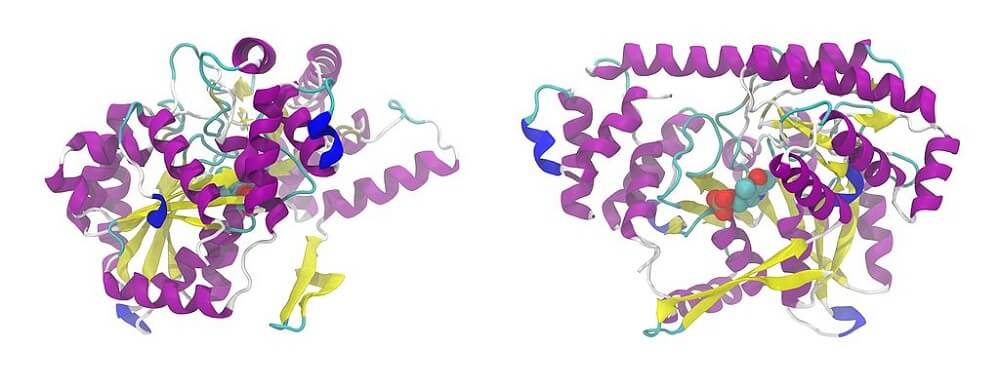
Alanine aminotransferase (ALT) is an enzyme coded by the ALT gene of chromosome eight in humans. It is the result of nearly five hundred connected amino acids. Gene expression for ALT production primarily occurs in the cytosol of liver cells (hepatocytes). It is also produced in the kidney, and in heart and skeletal muscle.

Alanine aminotransferase used to be called serum glutamic pyruvic transaminase (SGPT). It is measured for a specific liver function test and part of a liver panel. Alanine aminotransferase activity in the blood indicates that liver cells have been damaged to the extent that their membranes leak ALT into the blood circulation.
Alanine Aminotransferase Function
Alanine aminotransferase function is of great significance within the tricarboxylic acid cycle (TCA cycle). This is another term used to describe the Krebs cycle or citric acid cycle (CAC). All of these refer to the chain of reactions that produce cellular energy in the form of adenosine triphosphate (ATP). This reaction occurs within the cell mitochondria and is the foundation of cellular respiration.
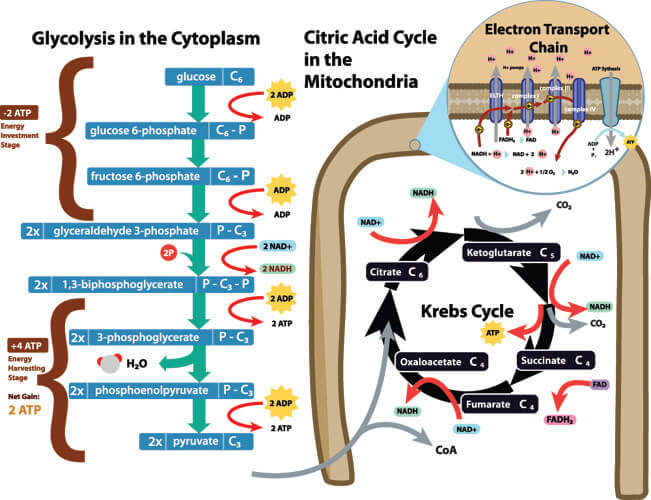
ATP is, more specifically, a catalyst within the transamination reaction. A transamination reaction is a reversible reaction that converts one amine into another. Amines are the most basic class of organic compounds and all contain nitrogen. The transamination reaction is the first stage of amino acid metabolism that ends in ATP production. As an amine, alanine aminotransferase is essential for cellular respiration.
With help from the coenzyme pyridoxal-5’-phosphate (vitamin B6), alanine aminotransferase enzyme speeds up the conversion of L-alanine and α-ketoglutarate into L-glutamate and pyruvate within the TCA cycle.
- L-alanine: non-essential amino acid; involved in sugar and acid metabolism, immunity, and energy production.
- α-ketoglutarate: a ketone derivative of glutaric acid; determines the rate of the citric acid cycle, protein synthesis, and protein degradation in muscle.
- L-glutamate: non-essential amino acid and derivate of glutamine; it serves as a fuel source and also acts as an important neurotransmitter – its role in the Warburg effect provides an energy source for cancer cells, especially in the brain.
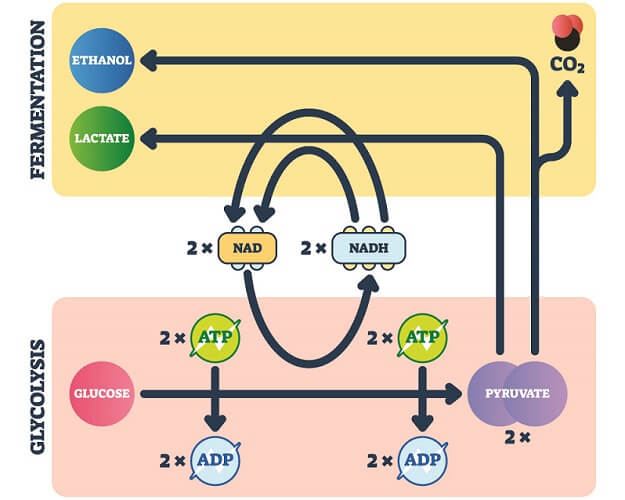
- Pyruvate: the result of glucose metabolism where one glucose molecule becomes two pyruvate molecules; these carry carbon molecules into the mitochondria for further processing. In the absence of oxygen, pyruvate undergoes fermentation to produce lactate – a less efficient source of cellular energy (see below).
Alanine Aminotransferase and Aspartate Aminotransferase
While alanine aminotransferase is primarily produced in the liver, aspartate aminotransferase (that also redistributes nitrogen between amino acids) is produced in high quantities in the heart muscle. Aspartate aminotransferase is also produced in the liver, skeletal muscle, kidneys, pancreas, spleen, lungs, and red blood cells.

When both ALT and AST levels are tested, results can indicate different pathologies. If both test results are elevated, liver pathology is usually diagnosed. If only AST levels are high and serum alanine aminotransferase levels are normal to slightly elevated, the most likely cause is a myocardial infarction; damaged heart muscle cells release AST into the circulation.
Most abnormal ALT results indicate liver malfunction. Slight elevations in both test results point either to skeletal muscle damage or the early stages of chronic liver disease.
Alanine Aminotransferase Test
An alanine aminotransferase test (ALT test) is usually carried out in tandem with an AST test. When hepatocytes are damaged, their membranes leak cell contents into the surrounding tissue. These contents are absorbed into the blood serum. By testing the blood of suspected liver injury patients, levels of ALT and AST can help with a diagnosis and subsequent monitoring of treatment. A normal AST:ALT ratio should be less than one.
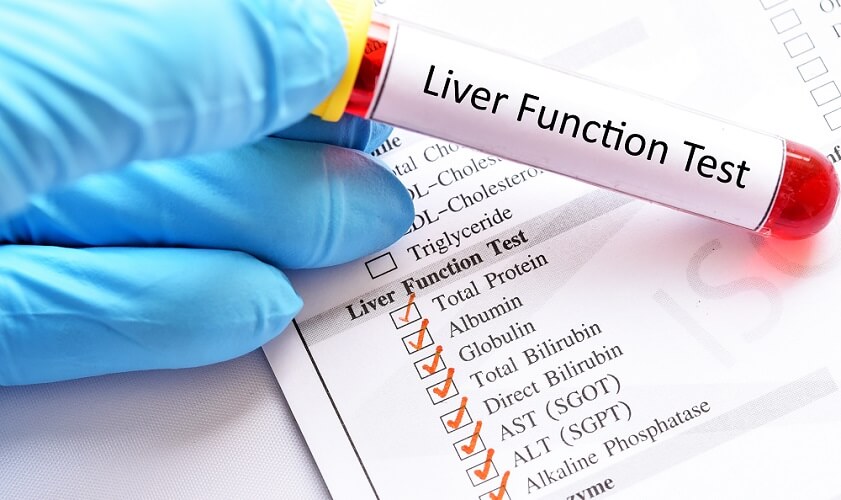
ALT is carried out as part of a liver panel when hepatic irregularities are suspected. A liver panel is composed of the following blood tests:
- ALT
- AST
- Albumin: a protein produced by the liver.
- Alkaline phosphatase (ALP) – a bile duct enzyme.
- Conjugated bilirubin: combined bilirubin inside the liver.
- Total bilirubin: all bilirubin in the blood.
- Total protein: all blood proteins, including antibodies and albumin.
Alanine aminotransferase range results are used solely to look at liver function and not to measure the efficiency of the Krebs cycle. It is only possible to test blood serum levels (not intracellular levels).
Many factors can temporarily or chronically affect our serum ALT levels:
- A high-energy workout can double ALT test levels when skeletal muscle (not the liver) releases it.
- When we sleep, our ALT levels decline.
- Gender, body mass index, and ethnicity can affect normal liver enzyme ranges.
- Alcohol abuse.
- Excess vitamin A.
- Drugs such as aspirin, statins (cholesterol regulators), and sleep medication.
- A range of pathological causes, primarily associated with liver damage

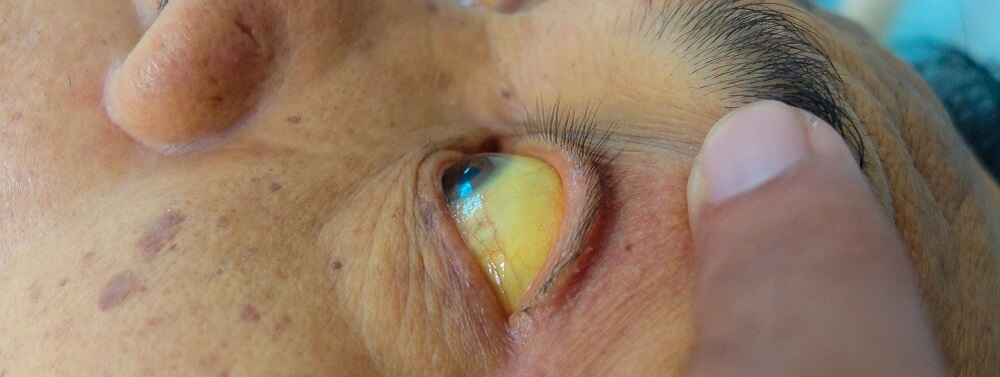
An abnormal ALT test result can indicate liver damage long before other symptoms such as jaundice, ascites, nausea, and vomiting appear. Abnormal liver enzyme results can precede the diagnosis of diabetes by many years.
Normal Alanine Aminotransferase Levels
The normal alanine aminotransferase range is 29 to 33 international units per liter in adult males and 19 to 25 IU/L in adult females. The above-mentioned non-pathological and pathological factors can positively or negatively affect these ranges.
You should not take part in a high-energy workout before going for an ALT test; the laboratory should also be made aware of any prescription or over-the-counter medication associated with raising or lowering liver panel results.

Low Alanine Aminotransferase Levels
Low ALT levels are associated with low total-body muscle mass and are often found in elderly or sedentary populations. Low alanine aminotransferase usually indicates both a degree of frailty and a healthy liver.
An alanine aminotransferase range of less than 7 IU/L is considered low. Causes in older and younger individuals are often nutritional; vitamin B6 deficiency is one common cause. Vitamin B supplements can return low ALT results to normal.

Smoking also lowers alanine aminotransferase levels in otherwise healthy populations. However, when liver disease is present, smoking has the opposite effect.
Regular workouts or higher-level physical activity can help to keep ALT results lower than normal over the long-term.
Chronic kidney disease is also associated with a lower alanine aminotransferase range. The worse the kidney function, the lower the serum ALT.
High Alanine Aminotransferase Levels
Chronically high ALT test results always indicate liver problems. The most common cause of high alanine aminotransferase is fatty liver disease. This is usually the result of excessive alcohol use and/or a diet high in saturated fat. Any result over 40 IU/L is considered high.

Nonalcoholic Fatty Liver Disease (NAFLD)
Too much fat stored in the liver cells can damage them. This is the most common form of chronic liver disease in the United States and affects up to 25% of the population. When a fatty liver becomes inflamed, the result is nonalcoholic steatohepatitis (NASH). This diagnosis causes further scarring that replaces normal liver tissue with scar tissue. Scar tissue is unable to function well and the resulting condition is called liver cirrhosis. The higher the percentage of scar tissue, the more cirrhotic the liver and the higher the risk of liver failure.
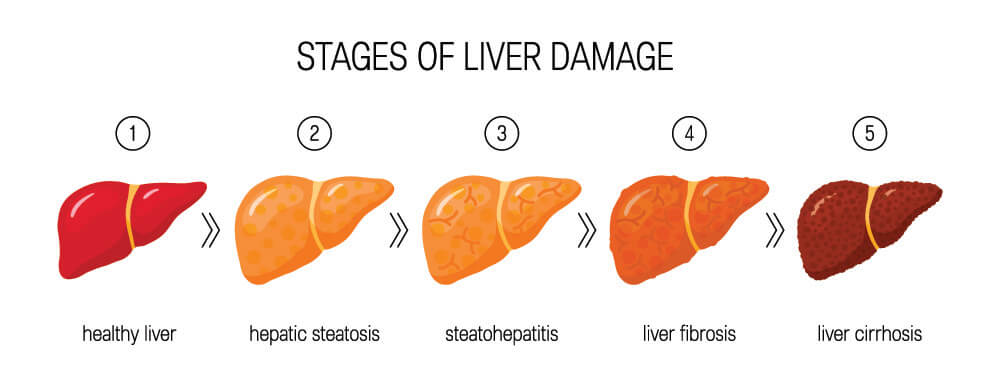
Alcoholic Fatty Liver Disease (AFLD)
As the name suggests, alcoholic fatty liver disease is caused by excessive alcohol intake. Alcohol abuse damages the liver in various ways and leads to a range of pathologies that include alcoholic hepatitis and alcoholic liver cirrhosis.
Risk factors for the development of AFLD must include chronic alcohol consumption. Drinking outside of mealtimes is an additional risk factor, as is gender (females), the presence of a hepatitis C infection, and vitamin A and E deficiency. These vitamins are necessary for hepatocyte regeneration.

You can find various alcohol unit calculators online that take into consideration your age and gender but little else. Low-risk drinking allows up to three units of alcohol per day for females and up to four units of alcohol per day for males. As a bottle of 13% wine contains approximately ten units, many people are unaware they drink more than the recommended daily limit.
Viral Hepatitis
Several viruses cause inflammation of the liver. The primary viral causes of elevated alanine aminotransferase levels are hepatitis A, B, and C. Today, most children are vaccinated against types A and B. As of yet, there is no vaccine for hepatitis type C.
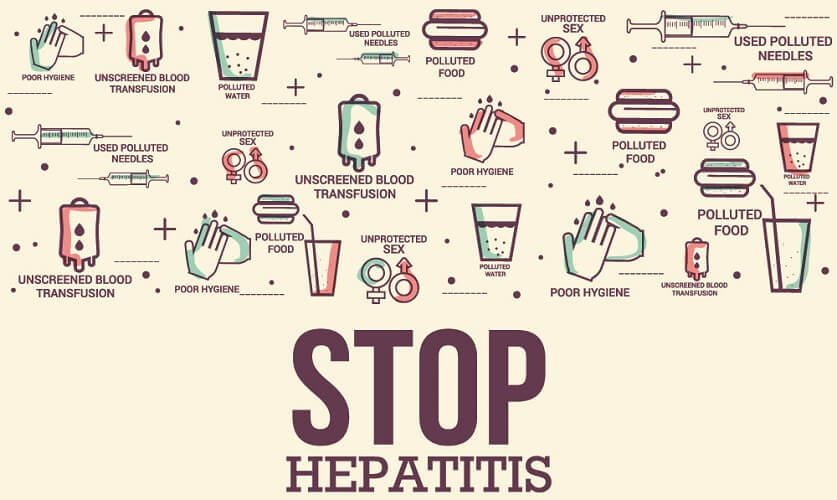
Hepatitis A is spread through infected fecal matter; B and C are spread via body fluids including semen and blood.
Autoimmune Hepatitis
When the body does not recognize the liver cells as part of the body, the immune system will begin to destroy them. The cause of this abnormal process is unclear but certain triggers have been observed. These include environmental factors and genetic factors. Autoimmune hepatitis can occur at any age and is more likely to affect females or those who have had contact with measle, herpes simplex, or Epstein Barr viruses.
As with all of the liver pathologies described here, long-term disease causes scarring of the liver tissue (cirrhosis) and low liver function.
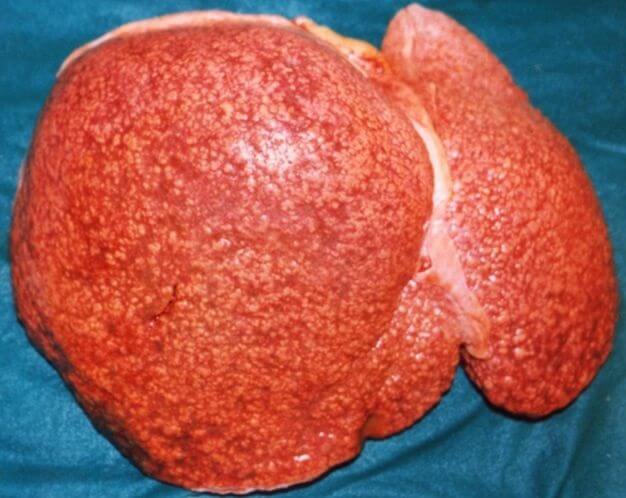
Drug Toxicity
Many drugs can increase alanine aminotransferase levels in blood serum but these elevations are usually asymptomatic. Liver function impairment as the result of medication is rare except in cases of overdose or chronic use.
Pain relief medication in the form of aspirin, ibuprofen, diclofenac, and acetaminophen can cause liver damage. Other drugs associated with increased liver enzyme tests (ALT and AST) are antibiotics, anti-epileptics, statins, cardiovascular drugs, and tricyclic antidepressants.
Hemochromatosis
Hemochromatosis or iron overload disorder is the result of iron absorption dysregulation; excess iron must then be stored in several tissue types, including the liver. Excess iron in the liver damages its functional cells, leading to cirrhosis and liver failure if left untreated.